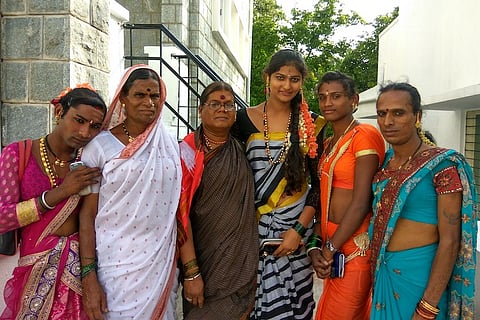
On a hot sweltering day, sitting in an unbelievably busy outpatient department at the ART (Anti Retroviral Therapy) centre of one of the largest government hospitals in Bengaluru city, I felt time stand still. Four trans women were sitting at my table – one a newly diagnosed patient, two already registered patients, and the fourth, a hijra elder who had accompanied the new patient for moral support.
The already registered patients had insisted on seeing me, in spite of the OPD queue being oppressively long on that hot summer day. "You treat us well doctor," said Meena*. "You check thoroughly and spend time." The second woman, Asiya, points a brightly painted finger at me and says, "You are the only person in this centre who actually touches us to see what health issues we have."
I remember feeling slightly embarrassed at this openly generous compliment, and also distressed – that what medical professionals should do as a matter of fact and a matter of routine, is becoming so rare that it is seen by patients as a favour rather than a right.
We are repeatedly told in medical college that the best clinicians are those who examine the patient and correlate different symptoms and signs with investigations to understand some of the complexity of how human bodies respond and react to disease, illness and healing. Physically examining a lymph node can throw up a variety of possibilities – the soft painful node suggestive of an infection, the rubbery, matted sensation of a tuberculous lymph node, the hard and painless lump suggestive of a more sinister malignancy.
Clinical medicine is often a physical relationship with one’s patient – the arm around a patient who has been socially ostracised is not just a random pointless action. It is a message to the patient that he or she is incredibly valuable and that the doctor is reaffirming this through touch. It is a message to the patient’s attenders that it is okay to touch and relate with an ill person and that an illness need not be a reason to completely devastate a person by physical and social ostracisation. It is also a message to the other patients who are often keen observers – a sort of role play, that every patient will be treated with respect and due courtesy.
Too often, one sees the medical profession insensitively refusing to touch patients who are different – poor patients, labourers, Dalits, people living with HIV, Adivasis, sex workers, trans communities, people with disabilities etc. The rejection is visible, harsh and painful without any pretensions or attempts at hiding. It is as though one can do away with basic courtesies with people who do not conform to one’s idea of acceptability.
In stark contrast, there is a great deal of interest, spilling well into the realm of the voyeuristic and impinging on human dignity and rights, when it comes to the sexuality of trans patients. Trans friends who have gone to the doctor for a cough or cold may not have a detailed history of their symptoms being taken, but a detailed history of their sexual life is a high possibility. “How do you have sex?”, “Do you have a penis?”, “Do you have sex with men or women?”, “Do you feel pleasure?”, “Do you feel pain?”, “What position do you have sex in?”
In addition, there often seems to be more of an eagerness to examine the genitalia of the trans person than of any other part of the body that is more likely to be related to the symptoms presented by the patient.
The recent parliamentary report on the Transgender Persons (Protection of Rights) Bill on the July 22, 2017, shows the same insensitivity and undue obsession with the genitalia of a person.
Dr Piyush Saxena, founder of the organisation called Salvation of Oppressed Eunuchs, seems to be the voice of the trans community without having any kind of credible basis for being considered so. In the Hindustan Times dated 11 September, 2017, the self acclaimed ‘magician’ and ‘past life regression therapist’, boasts of having “a sway with policy making about transgender issues for years” with whatever he has suggested being “accepted in toto!”
In the same article, the naive admission by Ramesh Bais, the BJP MP who is the chairman of the Parliamentary Standing Committee which gave a report on the Transgender Persons (Protection of Rights) Bill, that he doesn’t have much experience with transgender people doesn’t seem to prevent him from coming up with his own bizarre theories related to breasts and hormones, when he is not supporting similar bizarre theories by his ‘influential advisor’ Dr Piyush Saxena.
These influences are evident in the language of the Bill which seems to tend towards a genital mapping of the trans community with doctors prodding and poking into the most private parts of a person’s body, assessing their ‘sexual hotness’, the length of their clitoris and the nature of their orgasms and erections. This is an open invitation for the utmost violation of privacy and dignity that any citizen can be subjected to by a government and its systems. It will lead to trans people, who have lived with a chosen gender identity, being labelled as unable to meet some arbitrary criteria decided by people who don’t care either way.
The transgender community has no expert to thank beyond itself for its relentless fight to claim rightful spaces in society. From debilitating diagnoses of ‘psychiatric illness’, to physical, social and psychological abuse by an insensitive society, and obstruction of access to jobs and other social security measures, the community has seen it all. The high rates of suicide in the transgender community has to be taken serious note of – its impact not just on one individual, but on a larger trans community that sees suicide as an outcome of fights larger than what any one individual can handle.
The psychiatric Diagnostic and Statistical manual of Mental Disorders (DSM-5) in its fifth edition in 2013 took cognisance of the fact that a mismatch between one’s birth gender and identity were not necessarily pathological, and shifts focus from ‘treatment of an abnormality’ to ‘resolving distress over the mismatch’, dropping the loaded term ‘gender identity disorder’ to the more objective ‘gender dysphoria’. In India, the same benign view was taken by the Supreme court in the 2014 National Legal Services Authority (NALSA) vs Union of India case.
In the context of a trans man or woman, the role of a doctor and/or a psychiatrist is to ensure that the person who seeks or has been referred for help is able to deal with the psychological conflicts that comes with a socially imposed gender identity as well as to prepare for the medical and surgical transition to the gender identity that one opts for, if at all.
For the Bill to be truly sensitive, there is a need for policy makers and medical professionals to consult closely with a wide range of trans persons to understand that being transgender is not as simple as the absence or presence of particular sexual organs or functions, but a much more organic, diverse expansion of definitions and pre-conceived notions. It would lead to not just a Bill that ensures dignified living for the transgender community, but to a respectful learning by the others of the diverse definition of what being transgender means.
Listening with humility and genuine intent to learn (more importantly, unlearn) from a community that has created a new understanding of what gender means, is the only way forward for policy makers and medical professionals to make the trans Bill truly a recourse for the transgender community in India
The writer is a public health doctor and researcher who has worked on issues related to transgender health, rights and universal access to comprehensive healthcare. Views expressed are personal.