
The narrow lane dips and winds its way through Thiruvalluvar Nagar in Pallavaram. As thunder rumbles, and the overcast sky opens up, the half-naked children playing outside begin to run into dank little houses that jostle each other for space.
Across an open, festering gutter, a few houses are crammed into a compound. Mohammed Khasim greets us at the door of the first house. Inside, the spare, dark little room is crammed with men, women and young children. This could the abode of any of the thousands of people who come to Chennai seeking to eke a living. What sets this house apart is that it was once the home of Maimoon Beevi, the first person to undergo a heart transplant in a private hospital after the legalisation of brain death in India in 1994.
DECEMBER 3, 1967
CAPE TOWN, SOUTH AFRICA
In another part of the world, South African cardiac surgeon Christiaan Barnard made medical history when he did the first-ever human-to-human heart transplant in the world on December 3, 1967.The recipient was Louis Washkansky, the donor a 24-yearold woman called Denise Darvall, who was declared brain dead after being injured in a road accident. Washkansky died 18 days later but medical history had been made.
1968
MUMBAI, INDIA
In India, Dr P K Sen is credited with having done the first heart transplant in the country way back in 1968 at KEM Hospital, Mumbai, but the patient dies soon after. A paper on the first human heart transplantation in India is published by Dr P K Sen in the American Journal of Cardiology in December 1968. However, he first did experimental transplants on about 100 dogs, the findings of which were published in the Indian Journal of Research in 1965.
Dr Parulkar, who worked with Dr PK Sen on the dog experiments, recalls the transplant programme: “I was the backbone of that transplant programme. In 1962-63, Dr P K Sen told me, we have to start doing experiments whereby we must study the rejection of the heart, that is, when the heart is implanted in animals, how does it get rejected?”
So they started doing parasitic heart transplants, that is, transplants where the recipient’s heart was still present in the body. The surgeons would excise the heart of a puppy and attach it to the recipient’s dog’s neck, connecting the aorta to the carotid artery and the pulmonary artery to the jugular vein.
Dr Chris Barnard with Louis Washansky Image: https://www.westerncape.gov.za/general-publication/chris-barnard-performs-worlds-first-heart-transplant
Blood flowed from carotid artery of the recipient dog to the aorta of the puppy heart, perfusing the coronary arteries. This would make the heart begin to beat. The venous blood which came through the coronary sinus went back to the recipient dog through the jugular vein. “We devised a technique of covering the heart with the skin. The dog’s skin on the neck is very lax, so we easily covered the heart with the skin so that we could open and close it whenever we wanted to,” explains Dr Parulkar. A needle biopsy of the heart was taken till the organ was finally rejected by the recipient’s immune system.
Ultimately, we went to the real transplant, or orthotopic transplant, where you remove the recipient’s heart to do the transplant,” says Dr Parulkar.
The first human heart transplant was done by Dr P K Sen in 1968. Since brain death had not been legalised, the doctors knew that they would have to stick to the laws while carrying out the procedure.
“We had to accept the current definition of death, that is, when the heart itself stops beating. The donor’s heart had to stop beating before it was excised,” says Dr Parulkar, who was not part of the surgical team but remembers details of the surgery as he was involved in talks with Dr Sen. “So we came up with a procedure.”
This was first tested out on dogs. “The donor dog was given just sufficient anaesthetic so that he would stop breathing. He was kept alive on a respirator, as we connected a heart-lung machine to him through vein, and artery in the leg,” recalls Dr Parulkar. “On the other hand, we brought about a state of shock in him whereby his heart stopped.” Once the heart stopped and the ECG flatlined, one or two minutes had to tick by before they restarted the machine and the heart started beating again. ‘On this basis, we began tried to calculate the safe time that could elapse before the heart was revived. The period turned out to be anywhere from 15 minutes to 30 minutes,” recalls Dr Parulkar.
So, in 1968, when they received the first human patient came, the team was ready. “He was brain dead but his heart was beating,” says Dr Parulkar. “He was observed him for two days, the brain damage was extensive but they had to wait till the heart stopped and the ECG flatlined. The moment the heart stopped he was declared dead.
Since the heart-lung machine was connected to the patient, it was started just to ensure that the heart, when connected, would beat. One team began operating on the recipient, who had an enlarged heart and was in congestive heart failure. The second team excised the donor heart and immediately immersed it in ice-cold saline solution to keep the temperature of the organ as low as possible.
“The recipient was on a heart-lung machine. When and while he was on it, the major veins (vena cava) and the main aorta and pulmonary artery were clamped and heart-lung bypass, started. The advantage was that the whole body, every single organ except the heart, was getting the blood,” says Dr Parulkar. At that time, the heart was removed by cutting the aorta, pulmonary artery, and right atrium, even while preserving the sino-atrial (SA) node.
Finally, the recipient heart was excised, and the donor heart attached. “Suturing began from the left atrial border, left atrium to left atrium was the first connection. The second was right atrium to right atrium, and the third was pulmonary artery to pulmonary artery,” says Dr Parulkar.
The clamps were still on. After the last connection, aorta to aorta, was made, the clamp was removed, allowing the blood to gradually flow. The donor heart began beating in the recipient’s chest. Unfortunately, the patient died soon after the surgery but medical history had been made nevertheless.
By the 1970s, the heart-transplant programme in the country screeched to a halt. In fact, immuno-suppressant drugs to prevent the body from rejecting foreign organs are not available till the early 1980s.
AUGUST 3, 1994
NEW DELHI
However, change was in the offing. The Transplantation of Human Organs Bill 1992 is passed by the Parliament in May 1994, allowing the transplantation of organs from brain-dead patients. On August 3 the same year, Dr P Venugopal, head of the cardiothoracic centre in the All India Institute of Medical Sciences (AIIMS), leads a team of doctors in carrying out the first successful heart transplant in the country.
“Legislation of brain death happened in 1994 but the Bill was introduced in Parliament seven years ago and we knew it was a matter of time before it was passed,” says Dr P Venugopal. “So we had been working on the transplant programme for the past three years.” After the Bill is passed in May-June 1994, there are a few kidney donors but none who donates a viable heart.
On August 3, 1994, when they get a donor -a woman in her mid-30s who is declared brain dead, whose relatives are willing to donate her heart – they have a recipient ready in AIIMS, New Delhi. “The donor’s relatives were aware of organ donation, so they were ready. We had kept the recipient, a 45- year-old man, in the hospital for the past three months as we were preparing for a transplant,” says Venugopal. “Since the donor’s blood group was B+ve and the recipient was AB+ve (universal recipient), there was no problem,” says Venugopal. The operation goes off without a hitch, and the recipient lives for about 17 years.
Down south, in Chennai, yet another surgeon is striving to get a heart transplant programme going in MMM. On September 23, 1995, the D-day finally arrives.
SEPTEMBER 22
1995 CHENNAI
Thirty-year-old Hemalatha Soundarrajan is knocked down while crossing the road near Pallavaram. She is declared brain dead when rushed to hospital. Soundarrajan, a railway employee, is willing to donate her heart as they want her to live on through someone else. Soundarrajan, who is familiar with Cherian’s work and reputation, insists that he be contacted.
Vijaya Hospital: Cherian gets a call from Balaji Hospital, a trauma and accident hospital near Kathipara, saying a donor heart is available. Hema is soon shifted to Vijaya Hospital as he didn’t want her condition to deteriorate further. The search for a recipient begins. As the clock ticks, Cherian scours private hospitals in Chennai, Cochin, Trivandrum and even Hyderabad, looking for a suitable recipient in vain. Finally, he calls the General Hospital in Chennai.
General Hospital: Maimoon Beevi, 38, from Tambaram, who is suffering from dilated cardiomyopathy, has been waiting for a donor heart. Luckily, one of the most crucial factors has been taken care of. Since a transplant is the only option for her, doctors have been counselling her and she is ready to undergo the surgery. This is important because undergoing a heart transplant is also a highly emotional and traumatic experience. Writers and poets across languages have eulogised the heart, and linked it to love. Most people associate the heart with emotion and feeling, and wonder if having another person’s heart beating in your body will change you as a person.
Vijaya Hospital: Maimoon Beevi is brought to Vijaya Hospital. The formalities completed, Hema’s family leaves. The operation is fixed for 9 pm as the doctors want to conduct the procedure in the silence of the night when it won’t attract much attention. They don’t want the media glare or curious onlookers surrounding the hospital.
The Donor: Hema Soundarrajan, a resident of Chrompet and a Brahmin, and a mother of two daughters. Her husband and children are struggling to cope with the overwhelming blow life has dealt them, but certain that they want their wife and mother to live on.
The Recipient: Maimoon Beevi a Muslim, the wife of a vendor who sells handkerchiefs on the T Nagar platform. A housewife, she has been in and out of the government hospital, as her condition worsened. It was also the only place where she could get three meals a day regularly.
The Doctor: Dr K M Cherian, a Christian from Kerala, who has trained abroad. A well-known cardiac surgeon, the heart transplant is the biggest challenge he has faced so far.
MENTAL, INTELLECTUAL, EMOTIONAL AND PHYSICAL PREPARATION:
Only a few hours are left before the operation begins but years of training, and research kicks in and Cherian prepares himself mentally, intellectually and emotionally. If an operation is planned there is enough time to prepare – to discuss each step of the surgical procedure well in advance with his team. Social functions are avoided so that there is no temptation to drink.
But ‘firsts’ are always challenging and Cherian has come up with his own unique way to cope with the situation. “When you explain what has to be done to the patients or the relatives, they will always ask one question, ‘Have you done it before?’ So you should be prepared to answer that in the negative but also reassure them,” he says. “You have to tell them no one has ever done it before, in this country but all the steps have been worked out, your team is also prepared, and we know that we can do it. We are also undertaking this because there is no other recourse for you, no other choice in front of you,” he says.
Dr KM Cherian
On that September evening in Vijaya Hospital, Cherian gets ready to follow his own protocol. The strategy, or steps for the surgical procedure are worked out, then discussed threadbare with the team, which includes about six doctors, 4-5 nurses, an anaesthetist and a perfusionist.
Psychologically, from the moment he starts the procedure till he finishes, he completely forgets the fact that the procedure is being carried out for the first time. If he thinks it is something he is doing for the first time, or what others will say about it, nervousness will set in. So he simply doesn’t think about it.
Cherian has gone over the steps so many times in his mind that the procedure flows as if he has done it before. If you think it is something you are doing for the first time, or what others will say about it, nervousness will set in,” he says. “So I don’t think about it.”
VIJAYA HOSPITAL: SCRUB NURSE SRILATHA VASURAJ PREPARES
One of the senior-most scrub nurses, and one of Cherian’s most trusted aides Srilatha is alerted about the procedure. Cherian discusses with his team what he’s going to do, how he’s planning to do it, and what suture materials he needs. On the recipient team, Srilatha, with the help of others, cleans up, washes and sterilises the whole theatre. Nervous, she checks that all the equipment, instruments and drapes are re-sterilised.
VIJAYA HOSPITAL, 9 PM
The Procedure: Preparations for the surgery begin at 9pm. Hema Soundarrajan and Maimoon Beevi are wheeled into adjacent operating rooms. (This meant that, unlike other transplants later on, there is no delay in bringing the donor heart to the recipient.) There is an air of excitement fear and anticipation.
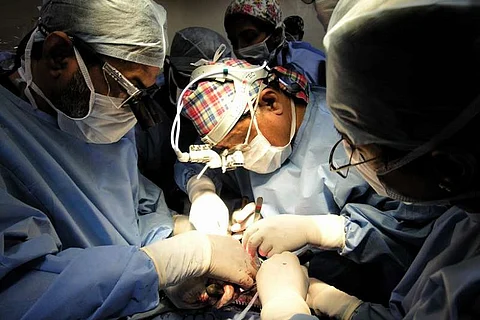
Hema’s heart is removed within 15 minutes, put in a basin full of sterile ice, and ‘prepared’ while Maimoom Beevi is initiated onto the heart-lung machine. When the basin enters the operating room, Beevi’s heart is removed. Diseased, it is huge, occupying more than half the chest cavity. Cherian begins the complex process of connecting the left atrium of Maimoon Bevi to the left atrium of Hema Soundarrajan, and right atrium of the Muslim woman to the Brahmin woman’s right atrium. The blood supply to the heart is resumed in a little over 40 minutes. As the team waits with bated breath, Cherian gently nudges the heart with the back of a forceps. The heart begins beating steadily, in perfect, harmonious rhythm. In the theatre, the team heaves a collective sigh of relief. It is the most exciting moment in their lives. The surgery, which began at 9pm, is over by 2am. The entire procedure has been completed in about five hours.
SEPTEMBER 23, 1995
VIJAYA HOSPITAL
At 2.30am, the patient is settled in into the ICU. Elated, Cherian calls his mother, unmindful of the late hour.
His mother picks up, anxious. “What happened?” she asks.
“I have good news for you. I just did my first heart transplant,” Cherian says, excitedly.
For Mariamma, it is a momentous occasion as her birthday has also just dawned. “It is the best present I can have from my eldest son on my birthday,” she says.
Back in the hospital, the ward boys garland Cherian. A cake is cut to celebrate the victory.
By morning, the news of the first heart transplant conducted in a private hospital in the country spreads.
A file picture of Maimoon Beevi with Dr KM Cherian
Even as Maimoon Beevi sits up in bed, having a light breakfast – a glass of milk and a piece of bread – Cherian readies himself for a press conference. Hema’s husband and children visit Maimoon Beevi. It is a highly emotional moment as the young girls meet the woman in whom their own mother’s heart beats.
Many would later cite the operation as a perfect example of religious harmony – when the heart of a Hindu was transplanted in a Muslim by a Christian doctor. “This was also highlighted by former President Abdul Kalam. I met him a year before he became the President and he asked me if there was any difference between the colour of blood of a Hindu or a Muslim,” recalls Cherian. “When I told him that blood has only one colour red, he said that it is something that we need to tell our politicians.”
Vijaya Hospital provided Beevi with immunosuppressant drugs for the first year free of cost. A friend of Cherian’s from Bahrain foot the bill for the next year. All her subsequent investigations were also done free of cost. “Every time she needed a check-up, we would go and pick her up,” says driver Bhaskaran, who is now a driver at FLL. “We were asked to be very careful while handling her.”
Six years later, Beevi complained of pain in the chest. The ECG showed changes and investigations revealed that the right coronary artery was blocked. An angiogram, and later, an angioplasty were done free of cost. After another six years, Beevi died after contracting urinary infection.
Hema’s family visited Beevi every year on their mother’s birthday. They would cut a cake and leave, happy in the knowledge that their mother’s heart still beats on. A few years later, they migrated to Australia. It is not known if they learnt of Beevi’s death.
SEPTEMBER 17, 2013
THIRUVALLUVAR NAGAR, PALLAVARAM
Maimoon Beevi’s two surviving sons – Mohammed Khasim, 48, and Abdul Khader, 32 – are aware of their mother’s place in medical history. But all that remains of her is a faded black and white photograph taken soon after her operation. With the passage of time, even the memories have taken on a sepia tint.
“My mother had a heart condition, her heart was too big,” says Khasim. Both he and his brother sell kerchiefs on the platform in T Nagar, like their father before them. “She was spending more and more time in the general hospital where she was admitted. We were told she needed a transplant but we had to wait for six months before we got a donor.”
He does remember the day when doctors informed them that Beevi had to undergo the operation. “She was scared, we told her to be brave, and the doctors also reassured us,” he says. For now, though her memories are lost in the passage of time. “We used to accompany her when she was called for functions. When Sonia Gandhi and Mother Teresa came to MMM, they met my mother along with then CM Jayalalithaa,” says Khasim. “But nobody speaks about her anymore.”
Hand of God: A biography of Dr. KM Cherian is published by Times Group Books