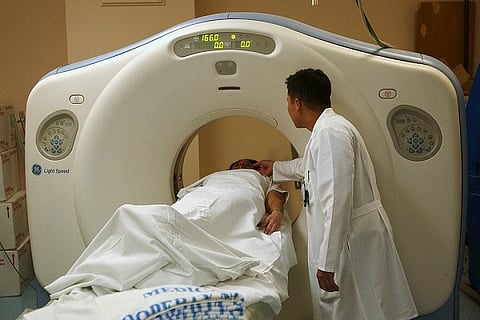

Computerised tomography (CT) scans are being increasingly used for medical diagnoses. In the UK, about 3m CT scans are carried out each year, and the rate per person is around five times higher in the US. However, concerns have been raised about the increased risk of cancer in people who have undergone these scans.
A CT scan (or “CAT scan”) provides doctors with a much clearer picture of what is happening inside the body than conventional X-rays. But they also deliver a much higher dose of ionising radiation. Ionising radiation causes tissue damage and can increase the risk of cancer. The increase in risk is proportional to the amount of radiation received.
Risk accumulates with repeated exposure, and children are more susceptible than adults. Because CT scans require many images to be taken in the same body area, they deliver more radiation than a conventional X-ray. For example, 50 times more radiation in the abdominal area has been detected. But a 50-fold increase in a very small number is still a small number.
It has been estimated that an abdominal scan delivers about six times as much ionising radiation as a person would receive from the environment in a year.
Authors of a large UK study found that children exposed to higher radiation doses from CT scans faced threefold increases in their risks of developing leukaemia and brain tumours compared with those who received lower doses. The higher the amount of radiation the children received, the greater their chances of developing these cancers were.
The number of children diagnosed with either cancer over a 17-year period was about 200 out of 180,000 who were scanned. About 170 of these 200 children would, according to the researchers, have developed cancer as a result of having had higher radiation exposure from CT scans. (They were chosen because the authors considered them to be most affected by radiation exposure.) The overall estimated risk was therefore 170 in 180,000, or about one in a thousand.
But there are methodological problems with this and similar research. Some 30,000 children could not be included in the data analysis, mainly because their medical records were incomplete, and their omission might have affected the findings. And, although the researchers attempted to do so, we cannot rule out “reverse causation”, that is, some children having had more CT scans because they had underlying health problems, rather than vice versa.
The researchers excluded children who were given CT scans because cancer was suspected.
As the authors acknowledge, this approach has limitations. Children who receive CT scans may differ from those who do not in unknown ways which also make the former more likely to develop cancer. The only way to definitively exclude reverse causation would be to do a randomised controlled trial. This would involve randomising children into higher and lower exposure groups and following them up over a long period to see how many in each group developed cancer. This would, of course, be totally unethical.
Also, the findings don’t exclude the possibility that children who have CT scans become at greater risk of experiencing other diseases, or over longer time periods than were considered in the study. Reverse causation might result in the risk from scans being overstated because the children who had more scans might have been more likely to develop cancers even if they had not been exposed to extra radiation. On the other hand, exclusion of other conditions and longer time periods might lead to the risk from scans being understated. Overall, there is considerable uncertainty about the risk estimates generated by the study.
Using UK data similar to that outlined above, researchers in the US concluded that about 2% of US cancers would be caused by radiation from CT scans. This conclusion is subject to the same cautions as detailed above. Also, the absence in the US of centralised databases of health records adds further complications to risk estimates.
If the estimate is approximately right, and current UK usage of CT scans in the UK is about a fifth of the US level, then about 0.4% of UK cancers would be caused by exposure to CT scans. Although readers may view this risk as acceptably low, it would mean that about 1,400 of the 350,000 annual new cancer cases estimated to occur in the UK would result from CT scans. Given the trend towards increasing medical usage, this rate can be expected to increase in the future.
Most experts believe that the risks associated with CT scans are greatly outweighed by their benefits. This conclusion might seem worryingly tentative. However, most decisions about risks entail value judgements because like is not being compared with like, in this case the clinical benefits of having CT scans to the additional cancer risk faced by those who undergo them, including otherwise healthy people.
Patients and parents offered a CT scan should ask their doctor to explain why it’s needed, and whether alternatives not involving exposure to radiation could be used.

Bob Heyman, Chair professor, University of Huddersfield
This article was originally published on The Conversation. Read the original article.